Chinese consensus on multidisciplinary diagnosis and treatment of gastroesophageal reflux disease 2022
Published 21 May, 2023
Gastroesophageal reflux disease (GERD) is a common condition in clinical practice, and results from the backward flow of stomach and duodenal contents into the esophagus and higher structures. Traditionally viewed as a digestive disorder, it was Professor Wang Zhonggao, a Chinese Academy of Sciences member, who drew attention to GERD's potential effects on the throat, mouth, nasal cavity, auris media, trachea and lungs during his own diagnosis in 2003. He initially sought medical help for severe "dyspnea" but it wasn't until he consulted with foreign colleagues that GERD was suggested as a possible cause. Despite treatment with standard anti-reflux drugs there was no improvement. To that end, he underwent laparoscopic surgery in the US—and brought about full recovery.
In order to make multidisciplinary care available for other sufferers of GERD, Wang established China's first ever GERD center in 2006 at the PLA Rocket Force Characteristic Medical Center (formerly the Second Artillery General Hospital). The center's establishment also marks the proposition of the model of multidisciplinary care of GERD for the first time in China. To further aid professional health care workers, in September 2019, the Society issued the first Consensus on Multidisciplinary Diagnosis and Treatment of Gastroesophageal Reflux Disease in China as a useful reference.
The 2022 Consensus was reached based on 72 statements, including the following:
- The concept of laryngopharyngeal reflux disease, gastroesophageal laryngotracheal syndrome and gastroesophageal airway reflux disease greatly extends the connotation of GERD, which is helpful to the development of multidisciplinary cooperation in GERD care;
- Patients with typical GERD-like symptoms are currently classified as erosive reflux disease, Barrett's esophagus, non-erosive reflux disease, reflux hypersensitivity, and functional heartburn types according to endoscopic findings, reflux monitoring results, and response to acid suppression therapy;
- Non-acid reflux is an important form of reflux on top of acid reflux, and the proportion of non-acid reflux events is often comparable to that of acid reflux, and in the case of acid suppression therapy may become the main form of reflux;
- Nocturnal gastroesophageal reflux (nGERD) symptoms are the main symptom in some patients with GERD, and nGERD is a common subtype of GERD and cause of refractory gastroesophageal reflux disease;
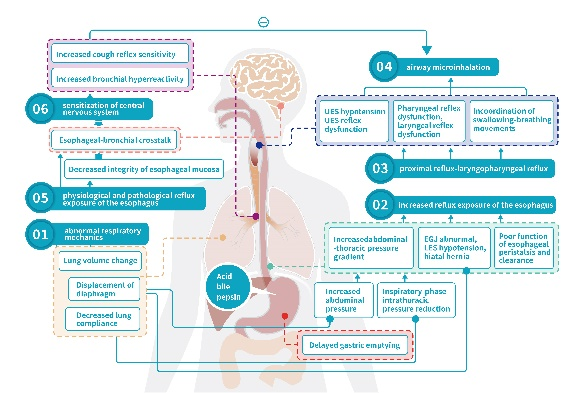
- Multiple sites and factors are involved in the occurrence of GERD, and the gastroesophageal junction is the major anatomically abnormal site that causes reflux occurrence;
- There are similarities and differences in the pathophysiological mechanisms of GERD in children and adults, and more attention should be paid to distinguishing between physiological reflux and pathological reflux;
- There is a higher prevalence rate of GERD in the elderly population, which is related to the decline of anti-reflux function caused by aging and other factors;
- Reflux monitoring, especially pH-impedance monitoring, can provide objective reflux parameters and clarify the correlation between reflux events and specific symptoms. It is the current "gold standard" for the diagnosis of GERD;
- GERD patients should be treated in a stepwise and staged manner. Treatment methods include lifestyle and diet adjustment, psychotherapy, Western medicine, traditional Chinese medicine, endoscopic treatment, and laparoscopic anti-reflux surgery. These methods target different levels, complement one another, and constitute a relatively complete anti-reflux treatment system; and
- The diagnosis and treatment results of GERD extraesophageal reflux syndrome obtained from different specialties should serve as feedback to the involved disciplines, so that all the disciplines can participate in the comprehensive care and accumulate experience for a virtuous cycle.
Image:
Contact author details: Jimin Wu, Department of Gastroesophageal Surgery, PLA Rocket Force Medical Center, drwujimin@qq.com
See the article: Zhuiwei Hu et al., Chinese consensus on multidisciplinary diagnosis and treatment of gastroesophageal reflux disease 2022, Gastroenterology & Endoscopy.