Want to avoid high-altitude sicknesses? Acclimatising in a low-oxygen level tent can help
Published 19 August, 2021
Prior to recent COVID-19 travel restrictions, the Earth’s mountains attracted millions of international tourists, trekkers, mountaineers and skiers each year. When travel restrictions ease, visitor levels are likely to return to their previous levels.
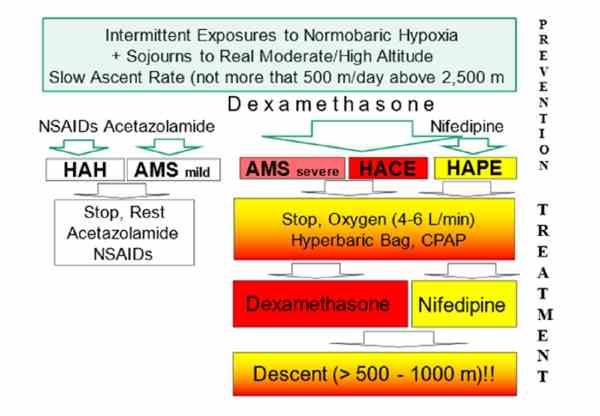
In a review published in the KeAi journal Sports Medicine and Health Science, a team of researchers from Austria and Switzerland examined recent study findings on the epidemiology and pathophysiology of high-altitude illnesses, along with options for prevention and treatment. These sicknesses include acute mountain sickness (AMS), high-altitude cerebral edema (HACE) and high-altitude pulmonary edema (HAPE).
In terms of pharmacological options, the team highlighted the unique effectiveness of dexamethasone, a medication used to treat rheumatic and lung conditions, among others. It was found to be effective in the prevention and treatment of almost all types of high-altitude illnesses, including AMS, HACE, and, more recently, the prevention of HAPE too.
In terms of non-pharmacologic prevention options, the review looked at modern pre-acclimatisation strategies that use simulated altitude in tents or rooms, which can be constructed at home. In a real altitude situation (hypobaric hypoxia) people experience low pressure and low oxygen. In a simulated altitude environment (normobaric hypoxia), only the oxygen levels are lower than normal.
According to lead author, Professor Martin Burtscher of Austria’s University of Innsbruck: “Although large scale studies are lacking, accumulating evidence from smaller studies and observational experience (including that of the authors) suggests that normobaric hypoxia is a promising and easy-to-apply tool for pre-acclimatisation before heading to high altitude.
“It not only helps to reduce the risk of high-altitude illnesses and maintain exercise performance, it also provides the attending physician with important information on (patho)physiological responses to hypoxia, the individual tolerability of hypoxia/altitude, and potential interactions between hypoxia and pharmacological treatment of pre-existing diseases.”
He adds: “A combination of normobaric hypoxia and high-altitude sojourns, e.g., for one or more days plus an overnight stay, are considered especially effective for pre-acclimatisation. A total of about 300 hours exposure to hypoxia (intermittently applied over several weeks) is generally viewed as the optimal level of pre-acclimatisation; however, every hour in hypoxia counts. Hypoxia exposures should be monitored by a physician and the severity of hypoxia should progressively increase, based on the individual’s well-being.”
The review also makes it clear that the “old” rules still apply; for example, ascending to high altitude slowly, listening to our bodies and understanding how to respond to signs of altitude sicknesses, including life-threatening forms such as HACE and/or HAPE.
Contact the corresponding author: Professor Martin Burtscher, martin.burtscher@uibk.ac.at
This study was made available online in April 2021 ahead of final publication in issue in June 2021.